For patients undergoing total knee arthroplasty (TKA), a combination of intravenous and periarticular corticosteroids does not improve pain control—but, may improve key indicators of functional recovery in the days after surgery, reports a trial in The Journal of Bone & Joint Surgery.
Intravenous (IV) plus periarticular (PA) steroids “yielded more significant improvements in the rehabilitation parameters,” such as knee movement and walking distance, according to the report by TCW Chan, MBBS, of Queen Mary Hospital, Hong Kong, and colleagues. “Thus, there was more robust evidence that corticosteroids enhanced functional recovery in the patients who received both PA and IV corticosteroids than in those who received intravenous corticosteroids only.”
Trial compares two routes of corticosteroid administration for TKA
TKA is a widely performed and cost-effective procedure, but many patients experience substantial postoperative pain. Previous studies have reported effective pain relief and improved mobilization after TKA with either IV or PA corticosteroid administration.
Chan and colleagues aimed to assess whether a combination of IV and PA corticosteroids could provide further improvement. In the new study, 178 patients undergoing initial TKA were randomly assigned to receive IV, PA, or IV plus PA corticosteroids. A fourth group received inactive placebo injections. All patients received standard opioid medications for pain.
Pain relief and key rehabilitation parameters were compared across groups. Patients and the researchers evaluating outcomes were both blinded to the treatment the patients received.
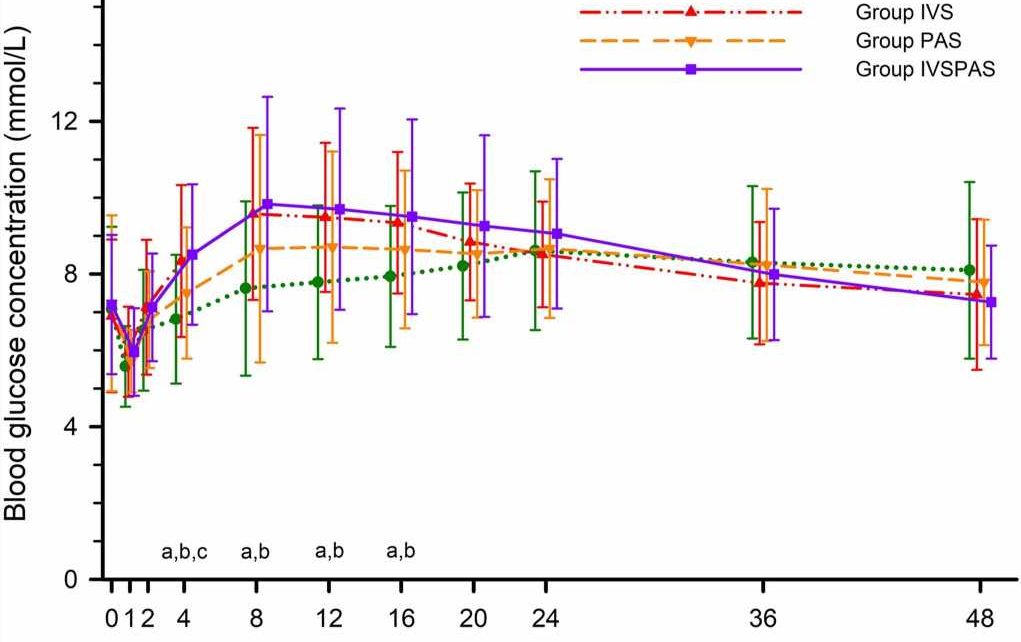
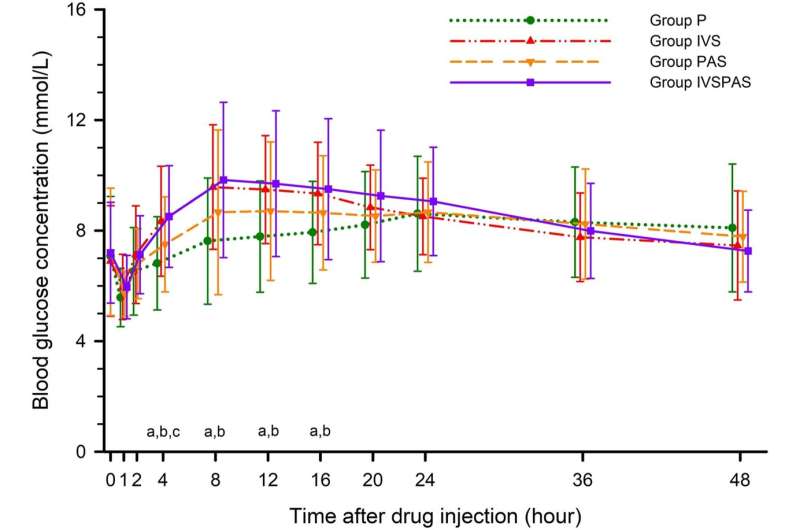
In first few postoperative days, pain scores at rest and during movement were significantly lower for patients who received IV corticosteroids, with or without PA corticosteroids, as compared with the placebo group. Patients who received PA corticosteroids alone had no reduction in pain scores compared with the placebo.
IV plus PA corticosteroids may enhance functional recovery
The combined use of IV plus PA corticosteroids led to improvement in several physical measures during rehabilitation. At three days, flexion in the operated knee was better for patients who received IV plus PA corticosteroids compared with the placebo.
The IV plus PA corticosteroid group also had greater quadriceps muscle strength and longer walking distances during the first three postoperative days, as well as higher scores on an elderly mobility scale. Some parameters, but not all, were also improved for patients who received IV or PA corticosteroids alone, as compared with the placebo.
Patients who received IV plus PA corticosteroids were also more likely to be discharged home from the hospital, rather than to a rehabilitation facility (67% compared with 38% in the placebo group). Rates of discharge to home were 55% with IV corticosteroids alone and 59% with PA corticosteroids alone.
The study confirms the role of IV corticosteroids in pain management after TKA, with significant reductions in pain scores and morphine use compared with a placebo. Adding PA to IV corticosteroids does not improve postoperative pain control.
However, the combined use of IV plus PA corticosteroids provided greater functional recovery immediately postoperatively. The researchers write, “These improvements in rehabilitation and recovery parameters may have contributed to the higher percentage of patients who were discharged home.”
Dr. Chan and colleagues conclude, “This study provides new insights into pain management in TKA that may enable better functional recovery and rehabilitation after TKA, and thereby advance the ability to perform arthroplasty as an outpatient procedure.”
More information:
P.K. Chan et al, Pain Relief After Total Knee Arthroplasty with Intravenous and Periarticular Corticosteroid, Journal of Bone and Joint Surgery (2023). DOI: 10.2106/JBJS.22.01218
Journal information:
Journal of Bone and Joint Surgery
Source: Read Full Article