Immunoglobulin A (IgA) deficiency is the most common primary immune deficiency worldwide, but its presentation has puzzled physicians and researchers. Some with the disorder present with symptoms like recurrent infections, autoimmune disease, or allergies, whereas others have no symptoms at all and only become aware of their IgA-deficient status through an incidental finding on a blood test. This variability has raised the question among researchers: Why aren’t many of those with IgA deficiency sicker?
A new study by researchers at Children’s Hospital of Philadelphia (CHOP) has begun to answer that question, demonstrating that IgA acts as a “tuner” that regulates the number of microbes the body sees every day, restraining the systemic immune response to these commensal microbes and limiting the development of systemic immune dysregulation.
“Right now, if we identify IgA deficiency in a patient through a blood test, we have no way of knowing whether the patient will become symptomatic if they aren’t already, and we don’t know whether or when they might go on to develop a more serious immune deficiency,” said Sarah E. Henrickson, MD, Ph.D., an assistant professor and attending physician in the Division of Allergy and Immunology at CHOP and co-author of the paper, which was published in Science Immunology. “Our paper lays the groundwork for being able to answer these critically important questions by providing a lens into how IgA and the microbiome interact and how an imbalance in that interaction could lead to symptomatic disease.”
IgA is an antibody protein that is part of the immune system and plays a role in fighting disease. It is found mainly in the respiratory and digestive tracts, but it can also be found in blood, saliva, tears, and breastmilk. To be diagnosed with IgA deficiency, patients must be over four years of age and have no IgA as determined through a blood test, as well as normal serum levels of IgG and IgM, without other known causes of immune deficiency.
Some researchers have suggested that perhaps IgM provides a “backup” role in some patients with IgA deficiency, explaining why some patients are asymptomatic. However, how secretory IgA and IgM work together in the mucosal system and whether their roles were redundant or distinct remained unclear.
To investigate this further, the researchers analyzed samples from 19 pediatric patients with IgA deficiency and 13 pediatric control patients, from 15 families, and they then complemented that analysis with studies of IgA deficient mice. They sought to answer two questions: how mucosal antibodies like IgA and IgM and system antibodies like IgG interact with mucosal microbes, and how IgA deficiency affects equilibrium of the immune system.
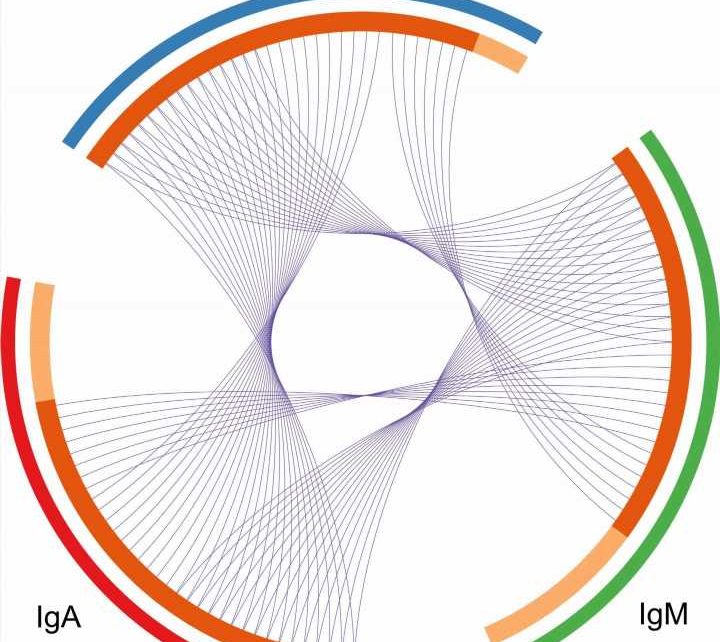
Analyzing both blood and fecal samples, the researchers measured antibody levels; identified the microbial targets of IgA, IgM, and IgG antibodies; and performed immune profiling to gauge the activation of the immune system. In doing so, they showed that although IgA, IgM and IgG target overlapping sets of microbes, the role of IgA is distinct from IgM in restraining commensal microbes in the gut, and IgM only modestly compensates for the absence of intestinal IgA.
They also determined that 26% of patients who were IgA deficient via blood tests had normal levels of IgA in their feces. Intriguingly, the patients with normal fecal IgA were less likely to develop immune dysregulation and clinical disease, as demonstrated through immune analysis of cytokine levels, whereas those deficient in both blood and fecal IgA were more likely to have elevated inflammatory cytokines and exhibit clinical symptoms.
To validate their findings, the researchers studied knockout mice who lacked IgA. Mirroring the findings in human patients, these mice exhibited elevated cytokines and immune dysregulation. The researchers also found live microbes in fat tissue of the knockout mice, which was not found in healthy control mice, providing further evidence for a role for IgA in modulating systemic microbial exposure.
“Based on these results, we propose that IgA supports the intestinal barrier to keep the proper balance of commensal microbes interacting with the immune system, acting as a tuner to keep the immune system in check,” said co-author Michael Silverman, MD, Ph.D. “Without IgA protecting the gut, commensal bacteria can get through, increasing a patient’s systemic exposure to these microbes and creating an inflammatory environment. Future studies with larger patient populations should investigate IgA levels in other target tissues and determine if these findings can be used to predict disease course and outcomes.”
More information:
Conrey et al, IgA deficiency destabilizes homeostasis towards intestinal microbes and increases systemic immune dysregulation, Science Immunology (2023). DOI: 10.1126/sciimmunol.ade2335. www.science.org/doi/10.1126/sciimmunol.ade2335
Journal information:
Science Immunology
Source: Read Full Article